Mental Health 301:
Obsessive Compulsive Disorder
by Lindsey Turnbull
May is Mental Health Awareness Month. This month can encourage us to change the perception of mental health and mental illness. So far, we have shared a general overview of Mental Health, and more focused looks at anxiety and depression, as well as eating disorders. If you have not read these articles, they are a great place to start. All information provided here is a general overview and not a substitute for medical advice from a licensed professional!
Today, we’re focusing on OCD. Obsessive compulsive disorder, or OCD, is an anxiety disorder that is
chronic and long-lasting, in which a person has uncontrollable, reoccurring thoughts (obsessions) and behaviors (compulsions) that he or she feels the urge to repeat over and over. – NIMH
Despite stereotypes, OCD is *not* a merely a preference for neatness or liking things orderly. It is a serious, chronic, and long-lasting mental health condition that requires professional treatment!
While 20% of the adult population reports having an anxiety disorder, about 1% of the population (2.2 million people) has OCD, and symptoms first appear in the teen years. Scientists do not fully understand what can cause OCD, although it includes genetic factors, brain structure, and environment. Someone who has experience abuse in childhood is at higher risk for developing OCD. Also, some people develop OCD after a strep infection. None of these things is your fault!
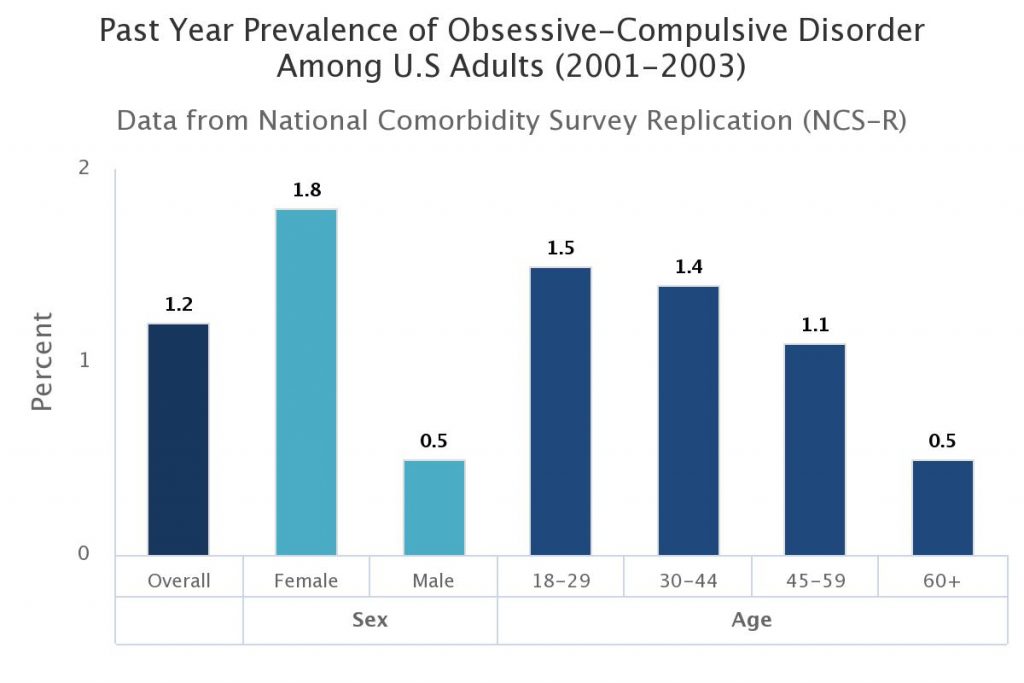
People with OCD may have obsessions, compulsions, or both. These symptoms interfere with aspects of life, like work, school, and relationships.
Obsessions are repeated thoughts, urges, or mental images that cause anxiety. These worries may center on the idea that something bad will happen, fear of contamination, fears of losing control, etc.. These thoughts are uncontrollable and recurring.
Examples of obsessions include concerns about cleanliness, fear of losing something, aggression, and a need for symmetry.
Compulsions are behaviors that one feels the urge to repeat over and over. These behaviors are like rituals that someone with OCD performs because s/he feels they will keep bad things from happening.
Common compulsions include checking/counting, hoarding, washing/cleaning, constantly seeking reassurance, and arranging.
Sometimes the obsessions and compulsions are related. For instance, someone with a fear of germs may wash her hands dozens of times per day. Other times, they are not related. A teen may feel like she needs to turn a light off and on a certain number of times to protect her from harm. OCD can overtake someone’s life.
Things OCD is NOT:
- Preferring things neat
- Handwashing
- Perfectionism
- An adjective (“OMG, I’m so OCD!”)
- Something someone can turn off or “just stop doing”
- A joke (“You have OCD? Come clean my room!”)
Signs of OCD in teenagers:
- Worries that seem irrational (i.e., worrying about getting sick when perfectly healthy)
- Worries that occur repeatedly
- Any type of compulsive action
- Distress when a compulsive action is interrupted
- An inability to explain a certain action (i.e., multiple hand washings in a row)
- Trouble concentrating, especially at school or when doing homework
- Losing friends or struggling to make friends
- Violent or disturbing thoughts that occur out of the blue
- Low self-esteem
- Getting in trouble at school for certain compulsive behaviors
These signs are not an all-inclusive, one-size-fits-all list. Symptoms of OCD can get worse during stressful times. Usually, someone with OCD knows that her worries are not logical. Sometimes teens with OCD do not realize that their obsessions and compulsions are excessive.
If you perform rituals or routines for 60 minutes or more a day, it is likely time to seek professional help.
Remember, OCD is a mental health condition. It is not something that will go away if ignored, nor is it something to be ashamed of. Anyone can have a mental health condition! It is best to get professional medical attention if you think you might have OCD or a related condition.
Someone with OCD may also have:
- an anxiety disorder
- ADHD
- Tourette’s syndrome (a Tic disorder that includes physical and/or vocal tics)
- Body dysmorphia (persistent and intrusive preoccupations with an imagined problem in one’s appearance, commonly focused on hair, skin, nose, chest, and/or stomach)
- Trichotillomania (a body-focused repetitive behavior, including hair pulling, skin-picking, nail-biting, etc.)
Getting a diagnosis is necessary for treatment. Many people with OCD report that therapy and medication are helpful in managing OCD. People with OCD live happy and successful lives! “Obsessive compulsive” is something someone HAS. It does not define you and all of the wonderful things you are and that you do!
More resources:
SAMHSA has a Behavioral Health Treatment Locator on its website that can be searched by location. You can also visit the NIMH’s Help for Mental Illnesses page for resources.
Taking charge of ‘bad thought’ OCD
The Ten Biggest Lies OCD Tells You, The Mighty
17 Quotes that Prove OCD is more than Being Neat, The Mighty
Black Emotional Mental Health Collective
The Trevor Project for Young LGBTQ Lives
National Asian American Pacific Islander Mental Health Association
National Alliance for Hispanic Health
Indian Health Service
You can also google “Teen Mental Health + your city” to find therapists who work with teens.
Related Reading
Mental Health 101: An Overview by Lindsey Turnbull
Mental Health 201: Anxiety and Depression by Lindsey Turnbull
Mental Health 202: Eating Disorders by Lindsey Turnbull
Mental Health 301: Obsessive Compulsive Disorder by Lindsey Turnbull
Mental Health 302: PTSD by Lindsey Turnbull
VIDEO: 5 Things NOT To Say When a Friend Opens Up About Mental Health
Leaders, Your Mental Health Matters Too by Julia Schemmer
The Portrayal of Mental Illness in the Media by Tracy Yu
Lindsey’s Story: May is National Mental Health Month by Lindsey Turnbull

3 thoughts on “Mental Health 301: Obsessive Compulsive Disorder by Lindsey Turnbull”